
 A picture is worth a thousand words, right? To a casual observer, the picture below is a young mother holding a brand new baby. To me, though, it’s a picture taken about an hour before I nearly died after giving birth to my second son…
A picture is worth a thousand words, right? To a casual observer, the picture below is a young mother holding a brand new baby. To me, though, it’s a picture taken about an hour before I nearly died after giving birth to my second son…
Maternal health is becoming quite a trendy topic to speak out about as more and more women come forward to share their experiences, but for so many of us, this isn’t trendy; it’s 100% real and 100% terrifying.
According to this info graphic from The Lancet, the USA has the highest rate of maternal deaths of any developed nation, while most other countries are seeing a steep decline in maternal deaths. For a nation with so many resources and so much knowledge, this information is absolutely bewildering. 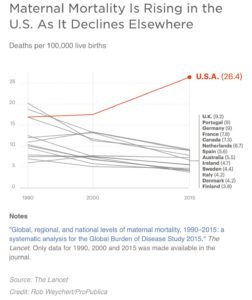
I remember the rush of emotions and the absolute exhaustion I felt after labor, coupled with the long list of instructions from my nurses: stay in bed until someone can help you up (because epidural), let us know if you’d like to eat something, and if you are bleeding more than one maxi pad per hour, call us. I had zero labor complications after my first delivery so I asked for a Diet Coke and a bagel, but also mentioned that I didn’t feel “right.” “Oh honey, no one feels ‘right’ after having a baby,” an older nurse sing-songed to me as she was leaving my room. “Let me know if I can get you anything else,” she said as she turned and walked away. “I don’t feel right,” I said again, but soon I just shelved my worries. I was fine because a medical professional was telling me I was fine. “People give birth every day, in worse places than this,” I told myself as I tried to focus on a re-run of Friends. “I am not on an episode of Grey’s Anatomy…I am not some weird exception…I am fine,” I chanted over and over again, taking sips of my Diet Coke and blaming my hormone changes and overall fatigue for my lightheadedness and inability to say things coherently. “I don’t feel good, I don’t feel right,” I said to another nurse a little while later, half begging her to ask me what I meant by “good” or “right” with my tone of voice. “It’s okay, let me get your nurse,” and then she too was gone.
A younger nurse I didn’t recognize came in and I repeated all my concerns to her: “I feel light headed, I feel weird, something is going on.” She pulled back the blankets on the hospital bed, and while shifting me to an angle that I was previously not sitting in, revealed the real issue.
I wasn’t over tired or super hormonal — I was hemorrhaging.
What I had waved off as being fine because I was being told I was fine, wasn’t fine. She stood me up and with that, I lost blood at a rate so heavy and so severe that my knees buckled and I fainted. (Later she would confess to me that she had to change clothes because she looked like “a scene from Kill Bill.”) Almost immediately, my son was taken out of the room as nurses and my OB/GYN ran in to administer shots to my thighs, bags of drugs and fluids, and started talking about transfusions. Thankfully, after several hours, I was under control enough to be moved into recovery. I delivered around 2pm and didn’t get to a recovery room until after 11pm. My rock star OB (seriously, I could write a blog series on THE MAN Roy Broady) came in to check on me and although he made some banter and jokes back and forth at the time, he told me later how urgent my situation was and that sadly, I am not alone.
According to a study by NPR, 700-900 women die in childbirth every year, with some 65,000 nearly dying.
American women die at a rate of six times the national average of other comparable countries, and African American women, low income women, and women living in rural areas make up a much higher percentage than anyone else. All this while infant mortality rates plummet to their lowest in history. The study found that a myriad of issues were to blame, but that primary focus on infant well-being, lack of preparation on what to do should a life threatening situation happen to a mother and not to the baby, poor coordination of care, and, just as in my case, waving away or diminishing a woman’s concerns about how she is feeling prior to delivery has led America to this crisis.
Listen, I am all for living babies you guys. If, while I was bleeding out in my hospital room that day, someone had said we can save you or your son, I would have told them to go to him instead. And I am immensely grateful to the nurses and to the doctor who rushed in that afternoon and began to put the procedures into place that would spare me from joining the statistics of fatalities listed above, but why did no one listen to me? This wasn’t my first delivery. Heck, even if it had been my first delivery, no one was in my body but me. No one could tell me how I was feeling other than me, and yet I let someone do just that and the result of that decision nearly cost me my life.
Nine months ago, I delivered another healthy baby boy, all the while crying in bursts and begging my nurses and that same doctor who I credit with saving me five years before, to please not let me die. No, I wasn’t being dramatic. I was actually, really, truly, may-as-well-have-been-held-at-gunpoint-in-a-bank-robbery-certain that I was going to bleed to death and die, especially since I was on blood thinning medication. I have a lot of words swimming around in my brain, but none of them can accurately describe the fear and total anxiety that I felt wondering at what point during the day I was going to literally bleed to death. (OB appointments are SUPER FUN when you ask your doctor to not let you die at every visit for 38 weeks, FYI.)



















It took almost 2 days for them to give me a blood transfusion after my hemorrhage, because my numbers looked good. Despite me feeling awful, unable to walk, unshowered after my water birth. I still remember the first time I laughed after my transfusion and thinking “I’ll be normal again”. My next birth was terrifying as well.
The ending made me full on ugly cry. I too nearly died at my first birth, even though my doctors were on the ball immediately and caught it early enough to avoid a transfusion, and were able to extract the retained part of my placenta in good time, I felt awful for days, just fading in and out of consciousness. 6 months ago, I delivered my second baby. I had a nurse stand at my side ready to stab me with a shot to help stop bleeding, and an IV ready in my arm to start up pitocin after baby was delivered. I knew I was going to be fine. But I still cried and told my nurses that I was scared, to please help me, not let me die. I’ll never be able to put into words just how scared I was. I spent that last half of my pregnancy completely terrified that I was going to die bringing my son into this world.